|
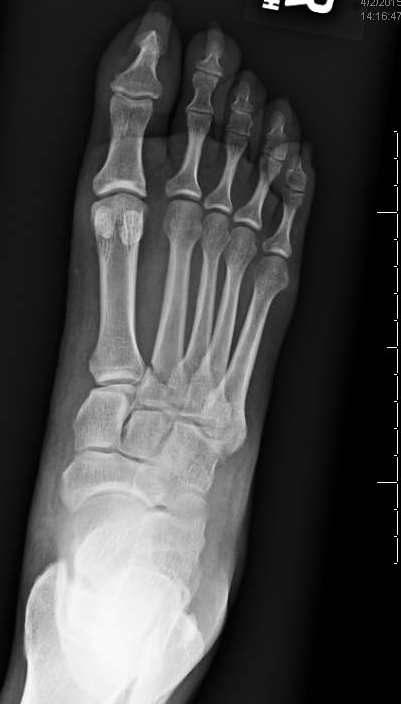
HPI: Middle aged female presents with right foot pain after "twisting" her foot. Physical Exam: Swelling present over the dorsum of the foot. No overlying laceration or abrasions. Palpable DP and PT pulses with intact sensation in SP, DP and tibial nerve distributions. Tenderness present over the base of the 2nd metatarsal. Unable to bear weight on RLE. Radiology: demonstrates oblique fracture at the base of the 2nd metatarsal Management:
We placed the patient in a well padded posterior leg splint and patient was instructed to not weight bear on her RLE. She was given follow up with orthopedics in 10 days for re-evaluation once swelling improves. Discussion:
0 Comments
HPI:
Middle age male with no significant PMH presents to the ED after amputating his right index distal fingertip. Physical Examination: Patient has a right transverse (slightly volar oblique) index fingertip amputation with distal tuft visible within the wound. The laceration grazed the nailbed. Sensation is intact in the radial/medial/ulnar distributions of the hand including throughout the index finger. Radial pulse is palpable and the finger has good capillary refill. Radiology: XR of right hand is notable for distal tuft amputation but negative for foreign body. Management: Approximately 1mm of the nail plate was removed exposing the edge of the nailbed. Soft tissues, including the fat volarly and the nailbed dorsally were elevated off of the distal phalanx. Distal phalanx was then rongeured until sufficient soft tissue could be mobilized to cover the bone. The soft tissue was then sutured close. The wound was covered with Xeroform and dressed. Ancef was given prior to discharge. Orthopedic follow up was arranged for the following day. Discussion:
HPI: Middle age man s/p MCC with open fracture of right leg. Tourniquet applied in the field. Physical Exam: Completely shattered tibia and fibula with 10cm open wound. Weak but palpable DP after taking tourniquet down. Intact sensation to light touch in superficial peroneal, deep peroneal, and tibial distributions. Able to wiggle toes and slight dorsiflexion. Management: Basic Management of Open Fractures
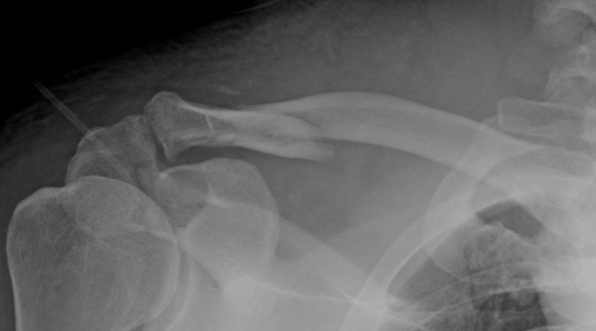
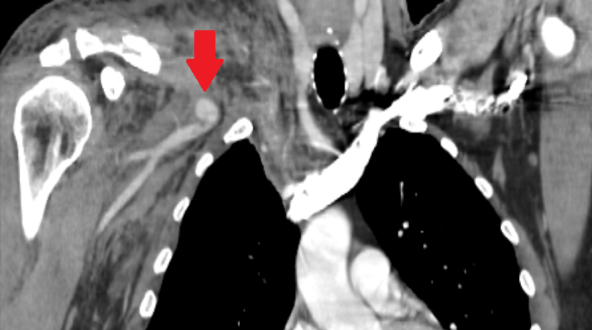
HPI: Middle age male who presented as an adult trauma code after a fall off a horse. Patient with significant pain in right shoulder and anterior upper chest. No numbness or tingling to the right upper extremity. No weakness to the right upper extremity. Physical Exam: significant deformity, edema, ecchymosis, tenderness to right clavicle. Normal strength with the exception of limited shoulder abduction secondary to pain on the right, normal sensation in the right upper extremity. Radial pulse 1+, biphasic on doppler on the right. Radial pulse 2, triphasic on doppler on left. Radiology: X-Ray Clavicle: oblique fracture of distal third of the right clavicle with inferior displacement of distal fragment. Associated R acromion fracture (see figure) CTA Chest: 12 mm right subclavian artery pseudoaneurysm, suspect right subclavian view transection. Right sided ribe fractures and pneumothorax. Management: Patient had a chest tube place, and was admitted to the STICU. Orthopedic surgery and Vascular surgery were consulted for his right clavicle fracture with underlying pseudoaneurysm. He underwent subclavian artery stenting by vascular surgery. In regards to his clavicle fracture, he was placed in sling for comfort, made non-weight bearing to right upper extremity. No operative intervention was performed.
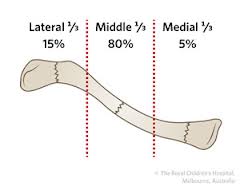
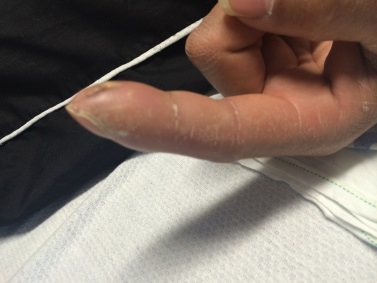
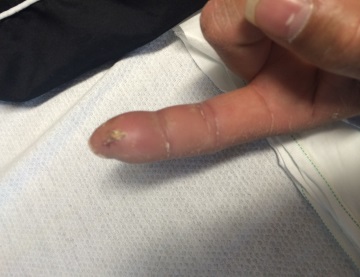
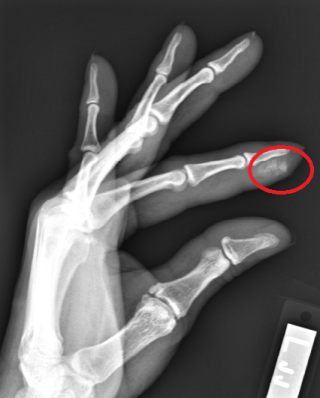
Discussion: Clavicle fractures are very common and account for 5-10% of all fractures. Vast majority of clavicle fractures are managed non-operatively and, with VERY few exceptions, nearly all clavicle fracture can be discharged to home from the ED with outpatient follow up if they, in the rare occasion, do require surgery. 80% of clavicle fractures involve the middle third of the clavicle. Without any associated neurovascular injury, these all can be discharged to home. Patient is likely to undergo outpatient surgery if there is greater than 100% displacement. The main associated injuries to rule out with clavicle fracture are: 1. subclavian artery/vein injury (suspect in patients with abnormal UE vascular exams, as presented in this patient case!) 2. floating shoulder, or scapulothoracic dissociation (suspect in patients with significantly widened or distracted fractures) 3. skin tenting (most patients, will have palpable deformity of clavicle with edema than may be confused for skin tenting—true skin tenting is when the skin is stretched to the point that is causes vascular compromise and skin discoloration) 4. pneumothorax (suspect in patients with significantly displaced clavicle fractures) HPI: Middle age male who presents with left index finger pain and swelling after injury involving high pressure paint spray gun. He has had increasing pain and swelling to distal portion of the finger since the incident 72 hours prior. Physical Exam: Edema, warmth, erythema and purple discoloration to middle and distal phalanx of left index finger. Tenderness to palpation. Unable to flex and extend at DIP secondary to pain. (See image). Afebrile. No other significant findings. Imaging: no fracture or dislocation. Increased attenuation in soft tissues below second distal phalanx (see image) Management: This patient had no fracture or dislocation and a relatively benign appearing exam. However, given mechanism of injury and high risk of underlying injury with high pressure injection injuries, patient was admitted to Ortho Hand Service. He was given clindamycin and tetanus vaccination. He was taken to the operating room for incision and washout. Significant damage to underlying fascia and tissue found with presence of white latex-type paint. Patient did well post-op with out complications.
Key Points:
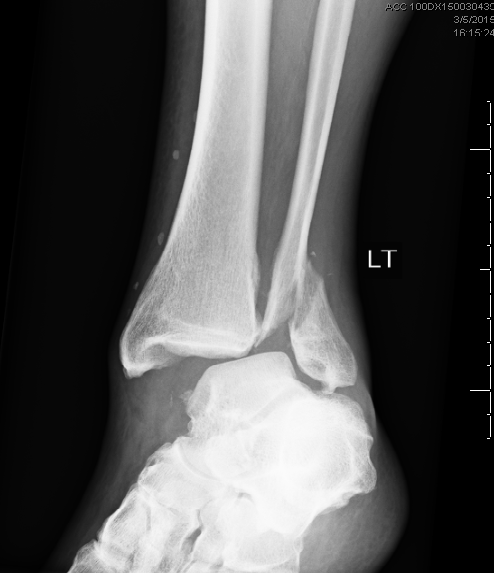
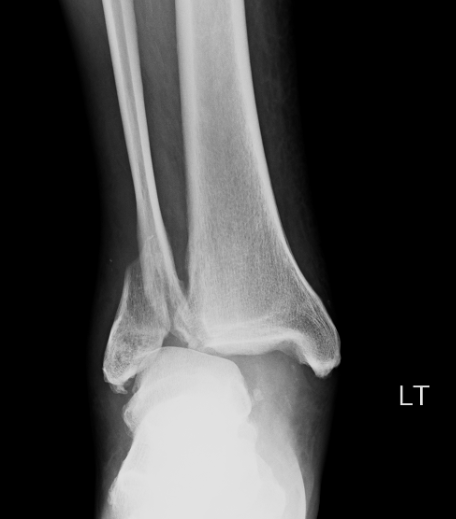
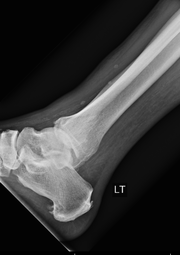
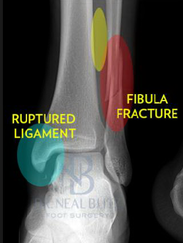
HPI: Middle age male who presents with left ankle pain, swelling, and deformity s/p fall down stairs. Unable to bear weight to LLE. Physical Exam: obvious deformity, edema, ecchymosis to L ankle. TTP over medial and lateral malleolus. Unable to flex and extend at ankle 2/2 pain. DP/PT 2+. Normal sensation to light touch to dorsal surface/plantar surface/1st web space. IMAGING: Diagnosis and Management: This patient has a Weber B distal fibula fracture with medial subluxation of the tibia and disruption of the mortise joint. Combination of distal fibula fracture and likely complete disruption of deltoid ligament is a bimalleolar fracture-dislocation equivalent. Thus, this is an UNSTABLE ANKLE! Patient’s ankle was reduced using axial traction and inversion, placed in posterior sugar tong splint. Injury required 3 reductions, which is common due to the instability of this injury. Patient was admitted to Orthopedic Trauma service and scheduled for next day ORIF.
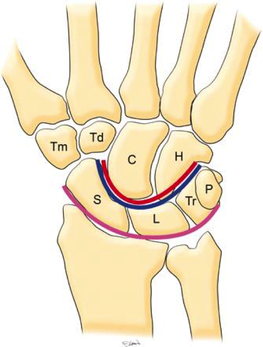
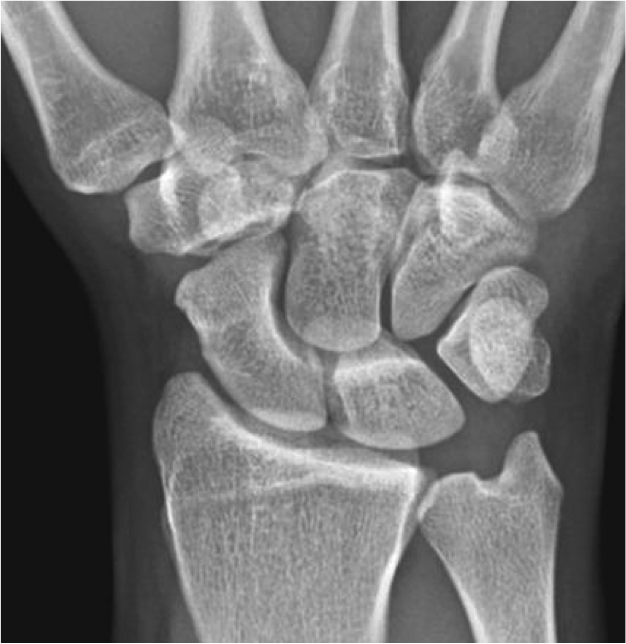
HPI: Young male presents after a fall while skiing with right shoulder and wrist pain. PE: Obvious deformity of the right wrist. No abrasions or ecchymosis. Full thumb abduction, able to flex at DIP and PIP joint of all 5 fingers, full abduction of all 4 palmar fingers, 5/5 strength to finger grip. Unable to range wrist, elbow or glenohumeral joint secondary to pain. Normal sensation to pinprick and two point discrimination of all five fingers. 2+ radial pulse with normal cap refill. Imaging: Anatomy: - Normal wrist anatomy consists of two rows of bones: o Proximal row: Scaphoid, lunate, triquetrum, pisiform o Distal row: trapezium, trapezoid, capitate, hamate - Ligaments of the wrist: o Interosseous ligaments run between the carpal bones and stabilizes proximal carpal bones. o Intrinsic ligaments insert and originate among the carpal bones to internally stabilize them. o Extrinsic ligaments connect radius and ulna to the carpus. How to make diagnosis:
Treatment: o Require emergent closed reduction and splinting into sugar tong splint.
Pearls:
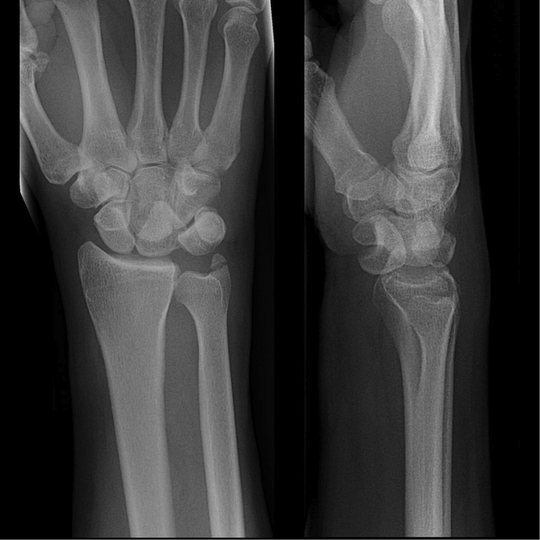
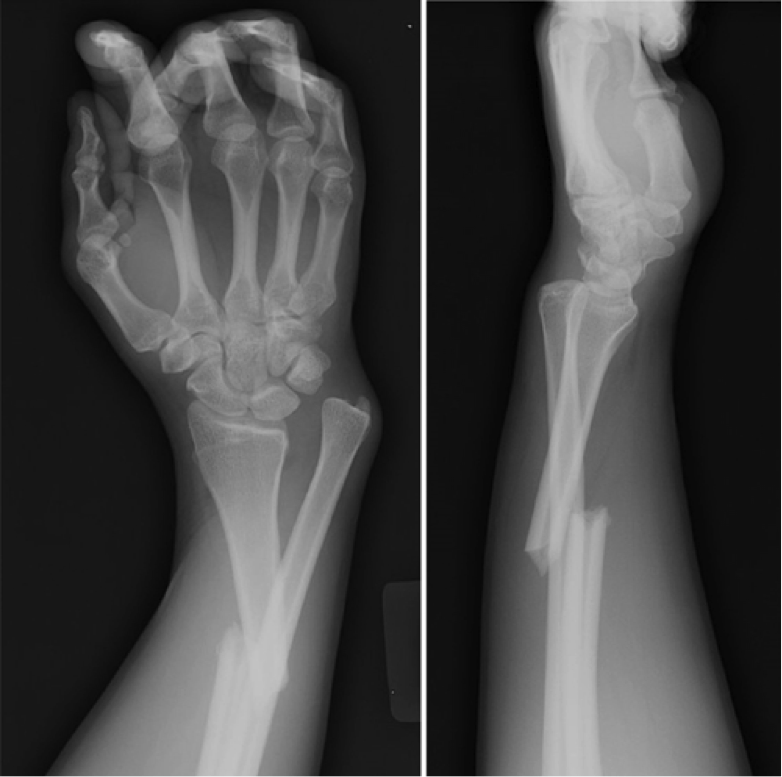
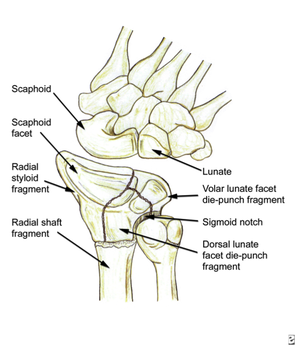
HPI: Adult male presents after being involved in a motor vehicle collision with right wrist pain and obvious distal deformity. PE: Obvious deformity of the right wrist. No abrasions or ecchymosis. Full thumb abduction, able to flex at DIP and PIP joint of all 5 fingers, full abduction of all 4 palmar fingers, 5/5 strength to finger grip. Slightly limited range of motion to flexion or extension wrist secondary to pain. Significant pain with pronation and supination. Normal sensation to pinprick and two point discrimination of all five fingers. 2+ radial pulse with normal cap refill. Imaging: How to Diagnosis: Radial shaft fracture and concurrent distal radioulnar joint. Most commonly seen in fractures of the distal 1/3 of the radius. Termed a Galeazzi fracture. Typically occurs secondary to direct wrist trauma (most classically dorsolateral) or with fall onto outstretched hand with forearm in pronation. Anatomy:
Treatment:
Pearls:
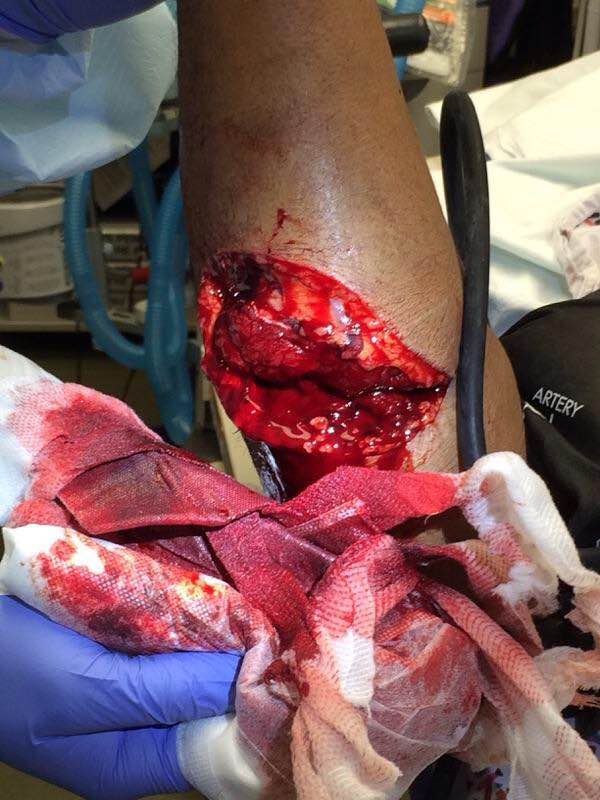
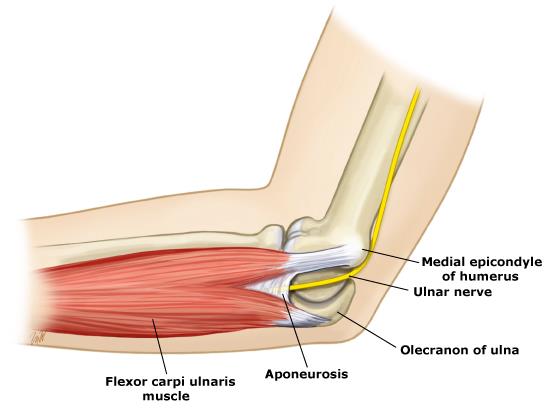
HPI: Middle age male who presents after falling at work. His medial forearm stroke a metal bucket just distal to his elbow and resulted in a large laceration. PE: Patient is unable to flex at the DIP of digit 4 and 5. He is unable to cross the second and third fingers or adduct his fingers. He has decreased sensation over the medial aspect of the 4th and 5th digit. Suspected ulnar nerve laceration. Anatomy: Derives from the medial portion of the brachial plexus (C8-T1). It lies posteromedial to the brachial artery in the upper arm and traverses behind the medial epicondyle. The ulnar nerve runs along on the ulnar aspect of the wrist along with the ulnar artery. It passes through Guyon’s canal where it bifurcates into sensory and deep motor branches. Innervation:
- Motor:
- Sensory:
Clinical conditions:
Treatment: Forearm exploration with transected nerve repair. Pearls:
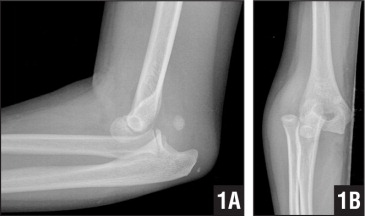
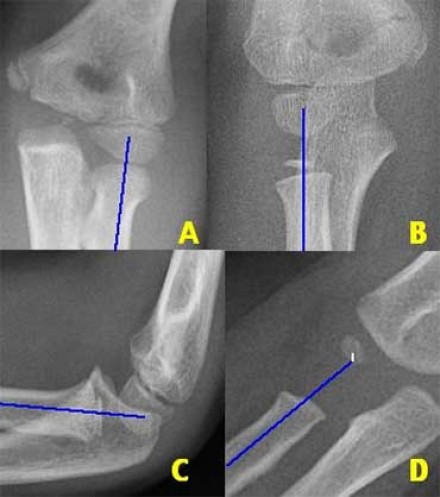
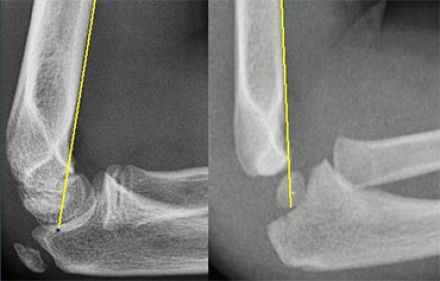
HPI: Pediatric male presents after a fall onto outstretched arm with obvious deformity to right elbow. PE: Patient is unable to cross fingers and has paresthesias in the ulnar nerve distribution. Initial radiograph showed posterior dislocation with questionable hyperdensity representing the medial epicondyle. We were unable to reduce under fluoroscopy as the medial epicondyle was more visible and the patient eventually required ORIF. Imaging: AP and lateral radiograph of the elbow Image 1: Showing associated medial epicondyle fracture How to Diagnosis: Two important lines help in making the diagnosis; radiocapitella and anterior humeral. Radiocapitellar line: Drawn through the center of the radial neck and should pass the center of the capitellum as shown below Anterior humeral line: Drawn through the lateral view of the surface of the humerus and should pass through the middle of the capitellum Ossification: 6 sites that fuse at different ages. Mnemonic = CRITOE
Treatment: Nonoperative with closed reduction and early range of motion (1-2 weeks) is most common. ORIF required for incarcerated medial epicondyle, inability to obtain close reduction, or significant instability. Pearls:
|
Orthopedics BlogAuthorCMC ER Residents Archives
June 2018
Categories
All
Disclaimer: All images and x-rays included on this blog are the sole property of CMC EM Residency and cannot be used or reproduced without written permission. Patient identifiers have been redacted/changed or patient consent has been obtained. Information contained in this blog is the opinion of the author and application of material contained in this blog is at the discretion of the practitioner to verify for accuracy.
|

 RSS Feed
RSS Feed
