|
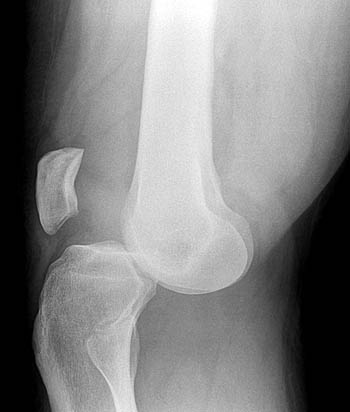
HPI: Otherwise healthy 27-year-old male who presents with right knee pain. The patient is a construction worker and while on a construction site today, a wooden wall fell onto him and other workers. The patient received an isolated injury to his right knee and presents with pain and deformity. Patient denies any other injuries, his vital signs are within normal limits. Exam: Patient lying in a supine position. Right knee has no significant effusion, erythema, or overlying abrasions/lacerations. Palpation of the right knee reveals a large step off between the patella and anterior surface of the femur. Patient is neurovascularly intact distally. Representative x-ray is shown below. http://radsource.us/ Discussion: There are 5 different types of knee dislocations based on the direction of displacement from the tibia.
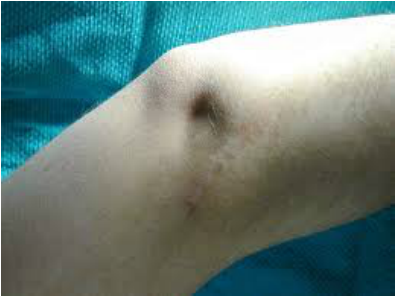
Physical exam often times result with no obvious deformity. It has been estimated that as many as 50% spontaneously reduce prior to arrival to the ED. In the emergency department, vascular examination is of utmost importance. With obvious deformity and absent pulses, reduction must take place immediately, before radiographs are obtained. After reduction, dorsalis pedis and posterior tibial pulses should be palpated, but the palpation of pulses does not rule out arterial injury. The next step should be measuring ankle-brachial index of the affected side. If the ABI is normal (> 0.9), then you can monitor the patient with repeat examinations as this has a 100% negative predictive value for arterial injury. If the ABI is abnormal (<0.9), then a CT angiography should be performed along with vascular surgery consultation. If pulses are still not palpable after successful reduction, immediate surgical exploration should be performed. There is one situation where reduction of the knee should not take place. The “dimple sign” represents buttonholing of the medial femoral condyle through the anterior medial joint capsule. The sign indicates an irreducible dislocation and closed reduction is contraindicated for the risk of skin necrosis. http://jbjs.org/content/87/7/1571
Initial imaging consists of plain radiographs. Remember, many of these reduce prior to arrival and the radiograph may appear normal. Despite this, you should look closely for avulsion fractures and osteochondral defects. CT angiography should be obtained as discussed above if necessary. After reduction and verification of ABI, the patient should be placed in a splint with 20-30° of flexion. Post reduction films should be taken after the splint or brace is applied to confirm placement. If emergent surgical intervention is not warranted, many of these require delayed ligamentous repair. Long-term complications consist of arthritic symptoms, instability of the joint, peroneal nerve injury, and chronic vascular compromise. Management Pearls:
References: 1. Patel, Anay. "Knee Dislocation." Orthobullets 08/11/15. Retrieved 10/15/15 from http://www.orthobullets.com/trauma/1043/knee-dislocation. 2. Peskun, C.J. et al. "Diagnosis and Management of Knee Dislocations." The Physician and Sportsmedicine. Dec, 2010. 4:38, pages 101-111. By Dr. Phillip Lunsford
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
Orthopedics BlogAuthorCMC ER Residents Archives
June 2018
Categories
All
Disclaimer: All images and x-rays included on this blog are the sole property of CMC EM Residency and cannot be used or reproduced without written permission. Patient identifiers have been redacted/changed or patient consent has been obtained. Information contained in this blog is the opinion of the author and application of material contained in this blog is at the discretion of the practitioner to verify for accuracy.
|

 RSS Feed
RSS Feed
