 1. Reflex examination is essential for the timely and correct diagnosis of Guillain-Barré Syndrome. 2. Diagnosis is based on clinical observations, however elevated protein in the CSF is present in 90% of patients suffering from Guillain-Barré. 3. The 20/30/40 rule is an excellent tool to guide decision making with regards to when to intubate patients suffering from this condition. 4. Be on guard for autonomic instability (heart rate, blood pressure, respiratory rate).
1 Comment
 1. TIME IS ESSENTIAL! Phase 3 & 4 IV tPA trial data and Phase 3 endovascular intervention data show a consistent association of improved stroke outcomes with earlier treatment. 2. The decision to withhold IV tPA treatment in the setting of mild or rapidly improving symptoms should be determined based on if any remaining deficits will be disabling for the given patient. 3. Randomized data suggest that isolated MCA occlusions respond similarly to either IV tPA or endovascular therapy. 4. The best available evidence suggests no absolute age cutoff for exclusion from IV tPA therapy within 3 hours of symptom onset. 5. Advanced age, hyperglycemia, and a high NIHSS (>20) increase the risk of hemorrhagic transformation for acute stroke treated with revascularization therapy. High Pressure Injuries - Surgical issue - Don't send them home! - Leave the finger alone - No Ice (decreases perfusion further)! - High risk for amputation Spontaneous Bladder Rupture- Extremely rare diagnosis - Expand your differential, use your diagnostic pause - Consider in pts with chronic GU issues - Add creatinine to abdominal fluid studies Heat Stroke- Temp >40 with AMS - Patients die from multisystem organ failure - Cooling and supportive care - Call Pearson for therapeutic hypothermia Nec Fasciitis and Ultrasound- Take time to ultrasound your patients
- Look for air (hyperechoic areas with shadowing), fascial thickening, deep fluid - Cannot rule out nec fasc with US  Steroids in meningitis - All cause meningitis - reduction in hearing loss and neuro sequelae ; nonstatistical reduction in mortality *** Pediatric - reduction in hearing loss and neurologic seuelae in Hflu; no recs in neonates *** Adult - decrease in mortality in strep pneumo - Steroids are thought to reduce CSF penetration of antibiotics *** Can be bad in resistant bugs - Don't give steroids after you give antibiotics Not everyone needs CT before LP IDSA rec CT - Age > 60, history of CNS disease (stroke, focal infection, mass lesion), immunocompromise, papilledema, altered level of consciousness, focal neuro deficit, new onset seizure within one week of presentation - may be too sensitive Newer data - documented normal CT that herniated after LP > newer recommendations - no LP if evidence of impending herniation Chemoprophylaxis for meningitis - Household contacts, school or daycare contacts, direct exposure to patients secretions - first line is rifampin, second line is cipro HSV meningitis - affects limbic structures of temporal and frontal lobes - 70% mortality untreated > 20% if treated with acyclovir - New psych symptoms or behavioral symptoms, cognitive deficits are more common - Seizures - CSF findings - pleocytosis with lymphocytic predominance, elevated RBC, elevated protein, > Beware that the CSF - can be normal in early disease process, can have neutrophil predominance, can have normal RBC, and glucose can be reduced Tuberculosis - Common in HIV patients - Indolent course then rapid progression - Suggestive CSF - clear appearance, lower pressure, < 50 PMN in kids, >30% lymphocytes in adults - Def give steroids in these patients Missed Dialysis & Syncope
- PR prolongation, QRS widening - can be a full block - Sine wave
RUQ Abdominal Pain
**** Can have ectopic pregnancy with declining beta****
Missed Pubic Rami Fracture
**** Fully examine your patients and document well & make sure to reassess****  1. Primary objectives of EM pregnancy US = IUP = midfundal GS with YS or fetal pole 2. Use your skills of depth, focus, frequency, and zoom to look for a YS or FP in a nice round sac in the middle of uterus. 3. Adnexa should be reviewed for ovaries, and then other. 4. Ovaries are medial to the internal iliac vessels and lateral to the uterus. 5. Don’t reverse your probe when doing transverse (coronal) views of the uterus and adnexas. Marker to the patient’s right leg. 6. Label images appropriately and delete the ones that are incorrect. 7. Finish your reports. Physicians outside our department are looking at them.  BASICS:
Stages of repair (Please look at the pictures): 1:Norwood: RV redirected to aorta (systemic). Shunt placed from RV into pulmonary artery as well (Sano shunt). Post norwood, patient highly fluid sensitive and high risk for clotting 2: Bidirectional Glenn (4-6 months): Connect SVC to pulmonary artery, disconnect RV from PA. 3: Fontan (1.5 - 4 yrs): Connect IVC to PA. Fenestrate IVC into the RV as pressure relief for the pulmonary artery. At this point pt is VERY fluid dependent, venous return is crucial for cardiac output. 
Surgical Setting: HTN, DM, Crush injury, open fracture, peripheral artery disease.
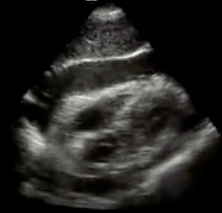 Etiology - Idiopathic is most common - Also: trauma, malignancy, infection, uremia, collagen vascular disease, hypothyroidism, etc Presentation - Dependent on rate of pericardial fluid accumulation - Symptoms: Sinus tach -> cardiogenic shock, distended neck veins, respiratory distress, Beck's triad - Work-up: EKG, chest x-ray, ultrasound (most important!) - Tamponade is a clinical diagnosis NOT an echocardiographic diagnosis, but US is a crucial adjunct Treatment - Definitive treatment = fluid removal (pericardiocentesis vs surgery) - Fluid resuscitation to increase preload - Avoid PPV and nitrates at all cost Indication for ED thoracotomy - Penetrating thoracic trauma, with witnessed signs of life (on arrival or en route), and less than 15 min of arrest w/ CPR Core Concepts: 1) Keep tamponade on your differential 2) Employ ultrasound early 3) Treatment = pericardial pressure relief 4) Fluid resuscitation can be life saving (increase preload)  Missed Foreign Bodies in Wound
Stenoclavicular Dislocation -
Chest Pain Pt seen with normal 12 lead ECG. D/C'd home. Returned within 12 hours with a STEMI. Core concept - LISTEN TO YOUR PATIENTS - history is everything - no amount of clinical decision rules can trump this. |
Archives
August 2018
Categories
All
|
 RSS Feed
RSS Feed
