 The basics of evaluation for elbow fractures in children are the same as adults - 2 (ideally 3) views, determine if there are any disruptions in the cortex, assess the radiocapitellar and anterior humeral lines (both should bisect the capitellum), and look for signs of hemarthrosis (anterior or lateral fat pads). Most elbow fractures in children are extension type supracondylar fractures. The Gartland classification system can be used to describe fractures:
The elbow is not fully developed until late adolescence. The timing of ossification center development varies from child to child, but girls generally develop slightly earlier than boys. The order of appearance IS reliable - use mnemonic "CRITOE" to remember the order:
Knowing the order of development can help you determine if that small piece of bone you're seeing is an ossification center or a bone fragment (comparison films of the contralateral elbow may prove helpful as well). A thorough neurovascular exam is the most important part of your assessment and will help determine management. For a quick motor exam:
Check a radial pulse, and assess color, temperature, and CAP REFILL. Pink and pulseless can be okay; pale and pulseless, however, is not. If you can't feel a pulse, listen for triphasic or biphasic Doppler flow. Type I fractures can be splinted in a posterior long arm splint with close Ortho follow-up Type II fractures can be managed like a type I if there is minimal displacement and swelling and the neurovascular exam is normal - otherwise splint and arrange urgent operative repair Type III will always require operative repair - emergently if a poor neurovascular exam, urgently if a normal exam
0 Comments

 1. ACS in the elderly can be tricky. Presentations can be subtle with the most common symptoms being chest pain, shortness of breath, diaphoresis and nausea. Patients > 65 who present without chest pain who have ACS have significantly higher mortality. 2. When making a diagnosis of DVT/PE consider why this patient is hyper-coagulable. Seek common etiologies and refer or admit for further workup if necessary. 3. Consider vascular surgery consult for large DVTs in proximal vessels in patient's with low risk for bleeding complications, as these patients may benefit from catheter directed thrombolysis or thrombectomy. 4. Signs of traumatic aortic injury include: widened mediastinum, abnormal contour of aorta, depressed left mainstem bronchus, deviation of NGT to right, loss of aortopulmonary window.  Before the Code
Recognize shock!
CT scan: A Dark and Lonely Place Where Trauma Patients Go to Die. - Be sure about your patient before they leave your side and go to the doughnut.  Shock: Recognition
 Submassive Pulmonary Embolism
Acute Retroviral Syndrome

 Internal Hernias
Osteomyelitis, MSSA bacteremia and pediatrics

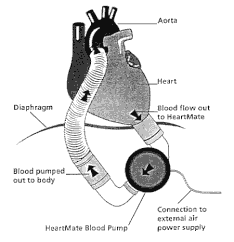 LVAD patient in ED = evaluate for (LVAD)2 L = Look, listen, and feel the LVAD device - Look: Connection & controller, green light with no alarm = good sign - Listen: For the hum of the LVAD, a quiet LVAD is BAD news - Feel: Hot LVAD controller = BAD, could mean distal obstruction, dislodgment, thrombosis V = Venous Thromboembolism, Ventricle - Venous Thromboembolism at greatest risk when INR < 1.5 with increased risk of TIA/Stroke and PE/DVT - Pump Thrombosis Signs = LVAD is hot, working hard, high RPM, low flow, dilated RV/LV, Low MAP - Right Ventricle: Signs of Right Heart Strain, RV failure is VERY concerning for LVAD patients, consider right sided STEMI, PE A = Anti-Coagulation, Arrhythmias - Anti-Coagulation: Bleeding risk from anti-coagulation and acquired von Willebrand syndrome (increased shear stress and decrease pulsatility of LVAD) = GI bleeds and head bleeds - Arrhythmias: check EKG on LVAD patients, can be in VF and still awake and talking, safe to defibrillate LVAD patient (if not emergent with consultation of LVAD team) D = Drive Line, Dehydration - Drive Line Infections: 40-60% of patients will develop an infection, also consider a deep pocket infection and obtain imaging to identify source of infection - Dehydration: Very common in patients as they adjust to not having to be fluid restrictive, leading to increased risk of suction events and arrhythmias, LVADs love FLUID |
Archives
August 2018
Categories
All
|
 RSS Feed
RSS Feed
