
0 Comments
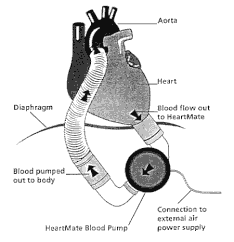 LVAD patient in ED = evaluate for (LVAD)2 L = Look, listen, and feel the LVAD device - Look: Connection & controller, green light with no alarm = good sign - Listen: For the hum of the LVAD, a quiet LVAD is BAD news - Feel: Hot LVAD controller = BAD, could mean distal obstruction, dislodgment, thrombosis V = Venous Thromboembolism, Ventricle - Venous Thromboembolism at greatest risk when INR < 1.5 with increased risk of TIA/Stroke and PE/DVT - Pump Thrombosis Signs = LVAD is hot, working hard, high RPM, low flow, dilated RV/LV, Low MAP - Right Ventricle: Signs of Right Heart Strain, RV failure is VERY concerning for LVAD patients, consider right sided STEMI, PE A = Anti-Coagulation, Arrhythmias - Anti-Coagulation: Bleeding risk from anti-coagulation and acquired von Willebrand syndrome (increased shear stress and decrease pulsatility of LVAD) = GI bleeds and head bleeds - Arrhythmias: check EKG on LVAD patients, can be in VF and still awake and talking, safe to defibrillate LVAD patient (if not emergent with consultation of LVAD team) D = Drive Line, Dehydration - Drive Line Infections: 40-60% of patients will develop an infection, also consider a deep pocket infection and obtain imaging to identify source of infection - Dehydration: Very common in patients as they adjust to not having to be fluid restrictive, leading to increased risk of suction events and arrhythmias, LVADs love FLUID 
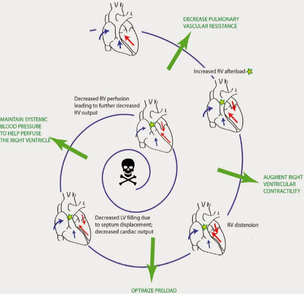 Right Heart Failure
Pulmonary Embolism in Pregnancy…and a PERC reminder
 1. Read with a specific focused question in mind. 2. Start by looking at the scientific abstract: Does the objective align with your question? Did the study answer its stated question? 3. Use the figures and tables of the results to get the “story”. 4. Use the discussion to glean the answer to the study question, how these results fit in the context of other work, the limitations of the study and conclusions. 5. The methods section provides a great starting template for future studies and allows for more in-depth analysis of the study. It’s not an essential read every single time.  Bed Bugs - Do not analyze a rash and simply call it bed bugs. There is a differential--includes scabies, fleas, bat bugs, dermatitis herpetiformis - Bite mark: occasionally linear formation where bedbug makes its "path." usually on exposed skin. erythematous wheel with occasional bloody center - 3/10 people bit will show NO symptoms. The skin changes that appear are an allergic reaction - They DO NOT transmit disease. Hep B, Hep C, HIV-- die quickly within the bedbug gut - They love warmth, dark and CO2. If bed bugs are seen in the well-lit ED, the patient likely has a MASSIVE infestation at home - Hitchhikers: they latch onto anything. at the laundromat, the hotel, your scrubs... - Oh not, not Diapause! Concept that bedbugs can remain without a meal for months and lie dormant. Even in cold as low as -12C. - Heat kills: Need 120 F for at least 30 minutes: kills all life forms. Dryer works. - Studies have shown "bug bombs" have no difference vs. controls - Treatment for rash: supportive. Rash generally resolves within 7 days spontaneously. Can use antihistamines or topical steroids PRN. However, antihistamines can make it difficult to discern if rash is bed bugs - Treatment at home: Combination of pest control, Heat, Sealing Cracks and Crevices, Treating Bed frames box springs and mattresses - Biopsy is of no use. ...now go change your scrubs  1) Afib RVR is often triggered by the same etiologies as sinus tachycardia. Before treating the arrhythmia, treat the most likely etiology. 2) In a person with normal cardiac function and structure, afib RVR is not the cause of the patients shock. Patients that are particularly sensitive to afib RVR include those with cardiomyopathies, recent MIs, severe diastolic dysfunction, HOCM, WPW, severe valvular disease, and severe coronary artery disease. In these populations, afib RVR often manifest as hypotension, pulmonary congestion, and possibly ischemia. 3) Procainamide should be the first line treatment in stable WPW with afib. AV nodal blocking agents should be avoided. 4) Review of recent literature suggest: - Diltiazem is more effective at controlling rate within 30 minutes when compared to metoprolol (Fromm 2015). - Beta blockers may have a mortality benefit when used in afib RVR & sepsis (Walkey 2016). - Use of a rate of rhythm controlling agent in ED patients presenting with an acute underlying illness results in an increase in adverse events compared to patients who did not receive rate or rhythm controlling agents (Scheuremeyer 2015). 5) Physicians should make an effort to optimize care and improve blood pressures before choosing a rate/rhythm controlling agent. Physicians should consider the patient's clinical status and comorbidities when selecting a treatment option.  Case 1 -- Hypotensive Inferior MI * Mmm bread and butter... Avoid nitroglycerin in the inferior MI. Preload! * Hypotension prior to RSI drugs? Bad. Crystalloid not helping? Pressors. * Make your FIRST attempt your best attempt. * Cath lab is a farther walk than anticipated... and may not have airway resources! * Be the leader: emphasize closed loop communication especially in code situations Case 2 -- NAT * Do not outsmart yourself. Do not talk yourself out of being suspicious for NAT. * No injury is 100% specific for NAT. Our job is to be sensitive, not necessarily specific. * Contact DSS! First encounter is mandatory reporter. Otherwise, story may change. * Just because DSS investigates and clears does not mean NAT is ruled out. * Be wary of your documentation: be objective, not a detective. Don't write things like "child consoled by mother after trauma"--remember, the victim often returns to the abuser * Like it or not, we all have inherent bias in the way we approach patients from various backgrounds. Be mindful of your assumptions. * Be on the same page and contact your colleagues: Social work, CHIPS, Child Abuse team, Trauma 
|
Archives
August 2018
Categories
All
|

 RSS Feed
RSS Feed
