|
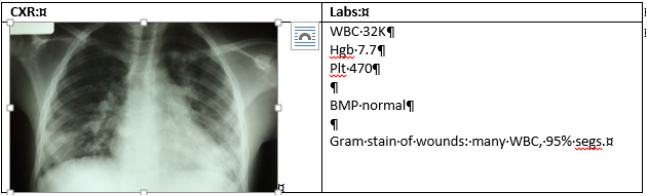
PEDIATRIC EMERGENCY MEDICINE BLOG Myositis Tropicans October 20, 2015 HPI: Previously healthy 14-yo M presents with fever, dyspnea, inability to bear weight, and draining abscess on left abdomen. Developed small abscess 1 week prior after seemingly negligible trauma, which older brother drained at home. Over next 5 days, developed inability to walk, spiking fevers, and severe dyspnea. No PMH. Lives at home with older brother. Both parents deceased. Physical Exam: Patient is sitting upright, severely distressed with tachypnea and heavily labored breathing. T 40, BP 110/70, HR 130s, RR 50s, SpO2 82% RA. Lungs: tachypneic with intercostal retractions and nasal flaring. Generally clear, but bibasilar diminished breath sounds. CV: tachycardic, hyperdynamic. Abdomen: distended and firm. Severe LLQ tenderness. Incised abscess on left abdomen with minimal active drainage, no erythema. Ext: severe pain with palpation of left thigh. Indurated. Pain with internal/external rotation. Unable to flex. Neuro: GCS 13-14. Clinical Course: HD 0: Formal incision and drainage of abdominal wound and empiric dicloxacillin. CXR as below. BiPAP. NS at 1.5 maintenance. Fever spikes > 39.5 despite drainage and antibiotics. HD 1: US of left hip/leg showed large abscess formation tracking upwards towards abdominal wound. I&D performed in OR. Continued fevers, now > 40. Antibiotics changed to vancomycin and clindamycin. HD 2: Hypotensive (90s/40s) requiring numerous NS boluses. 48 hours post second I&D, respiratory status improving, but new left elbow pain. HD 4: US demonstrates intramuscular abscess along proximal forearm. Taken to OR for I&D. HD 6: Blood pressure normalizing, fever curve improving. HD 8: Clinically improved. However, recurrent fever and mild left-sided chest pain and tachypnea. US shows left-sided pulmonary abscess. Surgical drainage planned. Discussion: This patient presents with classic findings of myositis tropicans (MT). MT is a disease most commonly encountered in the tropics, but there has been a steady rise in temperate regions.1, 2 It is characterized by skeletal muscle inflammation that leads to intramuscular abscess formation. The most common culprit is Staphylococcus aureus, accounting for 90% of tropical cases and 75% of temperate cases .1 Pathogenesis occurs in three stages: 1) Invasive – pain +/- fever without systemic symptoms; 2) Suppurative – abscess formation and systemic symptoms; and 3) Late stage – bacteremia and septic shock.3 Risk factors for development include trauma or strenuous exercise, and most importantly, immunocompromise. Diagnosis includes abscess aspirate or muscle biopsy for culture. However, approximately 15-30% of aspirates are sterile.4 Blood cultures, although recommended, are only positive in 5-10% of cases.5, 6 Imaging modalities such as US or CT/MRI are useful. Laboratory evaluation typically shows leukocytosis with left-shift, anemia, and thrombocytosis. ESR is elevated. Treatment is aimed at staphylococcus, and empiric therapy is dicloxacillin. Immunocompromised patients have higher risk for poly-microbial infection and should be covered accordingly. Recurrent fever is common due to new foci of infection. Repeat examination for new abscesses and subsequent drainage is essential. Treatment continues until abscess is clean, leukocytosis normalizes, and patient is afebrile x 7 days, usually 4-6 weeks.
Clinical Pearls for ED: * Consider myositis tropicans in any patient presenting with muscle pain, fever, and leukocytosis o Higher suspicion in patients who are from the tropics – specifically sub-Saharan Africa, Caribbean, and Asia o High suspicion in immunocompromised – HIV, poorly controlled DM, chemotherapy * Late presentation is common. Must consider in septic/bacteremic patients with multiple abscesses * Persistent fever typically means missed foci of infection – look for new abscesses, especially in children that have been treated elsewhere and are newly presenting to the ED * Incision and drainage is essential once abscesses have developed References: 1. Christin L, Sarosi GA. “Pyomyositis in North America: case reports and review.” Clin Infect Dis, 1992; 15:668-77. 2. Bonafede P, Butler J, et al. “Temperate zone pyomyositis.” West J Med, 1992; 156:419-23. 3. Chauhan S, Jain S, Varma S, Chauhan SS. “Tropical Pyomyositis (myositis tropicans): current perspective.” Postgrad Med J, 2004; 80:267-70. 4. Shepherd JJ. “Tropical myositis, is it an entity and what is its cause?” Lancet, 1983;ii:1240-2. 5. Gambhir IS, Singh DS, Gupta SS, et al. “Tropical pyomyositis in India, a clinic-histopathological study.” J Trop Med Hyg, 192; 95:42-6. 6. Brown JD, Wheeler B. “Pyomyositis: report of 18 cases in Hawaii. Arch Intern Med, 1984; 288:300-5. Author - JR Young
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
Pediatric EM BlogAuthorPediatric EM Fellows at CMC/Levine Children's Hospital. Archives
November 2016
Categories
All
Disclaimer: All images are the sole property of CMC Emergency Medicine Residency and cannot be reproduced without written consent. Patient identifiers have been redacted/changed or patient consent has been obtained. Information contained in this blog is the opinion of the authors and application of material contained in this blog is at the discretion of the practitioner to verify for accuracy.
|

 RSS Feed
RSS Feed
