
0 Comments
High Pressure Injuries - Surgical issue - Don't send them home! - Leave the finger alone - No Ice (decreases perfusion further)! - High risk for amputation Spontaneous Bladder Rupture- Extremely rare diagnosis - Expand your differential, use your diagnostic pause - Consider in pts with chronic GU issues - Add creatinine to abdominal fluid studies Heat Stroke- Temp >40 with AMS - Patients die from multisystem organ failure - Cooling and supportive care - Call Pearson for therapeutic hypothermia Nec Fasciitis and Ultrasound- Take time to ultrasound your patients
- Look for air (hyperechoic areas with shadowing), fascial thickening, deep fluid - Cannot rule out nec fasc with US  BASICS:
Stages of repair (Please look at the pictures): 1:Norwood: RV redirected to aorta (systemic). Shunt placed from RV into pulmonary artery as well (Sano shunt). Post norwood, patient highly fluid sensitive and high risk for clotting 2: Bidirectional Glenn (4-6 months): Connect SVC to pulmonary artery, disconnect RV from PA. 3: Fontan (1.5 - 4 yrs): Connect IVC to PA. Fenestrate IVC into the RV as pressure relief for the pulmonary artery. At this point pt is VERY fluid dependent, venous return is crucial for cardiac output. 
Surgical Setting: HTN, DM, Crush injury, open fracture, peripheral artery disease.
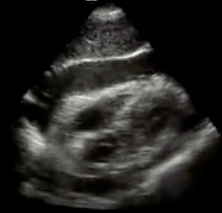 Etiology - Idiopathic is most common - Also: trauma, malignancy, infection, uremia, collagen vascular disease, hypothyroidism, etc Presentation - Dependent on rate of pericardial fluid accumulation - Symptoms: Sinus tach -> cardiogenic shock, distended neck veins, respiratory distress, Beck's triad - Work-up: EKG, chest x-ray, ultrasound (most important!) - Tamponade is a clinical diagnosis NOT an echocardiographic diagnosis, but US is a crucial adjunct Treatment - Definitive treatment = fluid removal (pericardiocentesis vs surgery) - Fluid resuscitation to increase preload - Avoid PPV and nitrates at all cost Indication for ED thoracotomy - Penetrating thoracic trauma, with witnessed signs of life (on arrival or en route), and less than 15 min of arrest w/ CPR Core Concepts: 1) Keep tamponade on your differential 2) Employ ultrasound early 3) Treatment = pericardial pressure relief 4) Fluid resuscitation can be life saving (increase preload)
Case 2 - Ludwig's Angina- Ludwig’s angina is infection within the sublingual/submandibular potential space, isolated by superficial fascia. Infection demonstrates rapid progression with posterior deflection of the tongue, obstructing the airway. - Airway management, ENT consultation and IV antibiotics (penicillin + metronidazole, clindamycin or ampicillin/sulbactam) are the necessary steps for management of Ludwig’s angina. Severe Mucositis- Mucositis is a common side effect of most chemotherapy and head/neck radiation regimens that is associated with significant morbidity. - Severe mucositis carries 75% risk of serious co-infection and 9% risk of associated mortality. Ehler's-Danlos and Aortic DIssection- Ehler’s-Danlos Syndrome, an inheritable collagen vascular disease, is associated with hyperextensible skin and hyperflexible joints; many subtypes are at risk for arterial aneurysm, dissection or rupture at young ages.
- Management of acute aortic dissection or perforation includes vascular surgery consult (for emergent intervention) and decreased BP/sheer stress with IV nicardipine or esmolol.  Staph Aureus Infections - Hospital acquired infections relatively stable over the past 5 years - Community acquired infections on the rise - One ED visit increases risk 4-fold - Protect your patients! - Patients on hemodialysis have a 50-180 fold increased risk for developing infective endocarditis … be wary the vague presentation of endocarditis! Globe rupture: - Protect without pressure! - Prevent vomiting/valsalva - Don’t forget your tetanus - Avoid ultrasound (just don't tell Dr. Tayal) Hypocalcemia: - Potassium is not the only electrolyte that causes rhythm disturbances - When facing new EKG changes, consider magnesium and calcium  ** The New Code Cool is being launched across our system. ** Focus on: Cooling times, resuscitation, hemodynamic management, ventilator management. ** Literature supports cooling to either 33C or 36C; we will continue to cool to 33C pending additional ongoing studies. 1. Use new “Code Cool – Induction” order set. 2. Activate Code Cool via PCL line (essential for nursing resources, ICU bed allocation, and patient tracking). 3. Consult cardiology and intensivisits on all Code Cools. 4. Cool to 33C unless intolerance to cooling (dysrhythmia), sepsis, or bleeding, then cool to 36C. 5. Induce cooling with ice packs, cold fluids 30cc/kg, and long-acting neuromuscular blockade (vec 10 mg IV) 6. Goal MAP > 70 mmHg at all times (> 80 mmHg if chronic HTN) 7. Treat blood pressure aggressively with norepinephrine (not dopamine) 8. Titrate FIO2 on ventilator down to 40% if possible while maintaining O2 sat > 95%. 9. Code Cool/STEMI: Activate Code STEMI also with age < 75, downtime < 20 min; others discuss immediately with intensivisits; don’t delay cooling. 10. Don’t delay initiation of cooling for CT imaging. Recall, few VF/VT arrests (< 5%) are due to PE.  Transplanted organs - don't act like normal organs - won't hurt and are in weird locales RAID - Potential Complications to Consider Rejection - Hyperacute - w/in minutes - we won't see - Acute - Chronic Anatomy - Vascular - stenosis, aneurysm, thrombosis - Nonvascular - leak, scar formation, dislodged stint, stone formation Infection - First 28 days - nosocomial - 1-6 months - viral infections - CMV, hepatitis, EBV, HH6; oppurtunisitcs - PCP, listeria, fungal - > 6 months - Healthy - UTI, PNA, cold, Chronic viral infection - EBV, zoster, HSV Drug Toxicity - Transplant immunosuppressants - cyclosprine, tacrolimus > can hurt the kidneys; - Imuran, cellcept - hematologic effects - Lots of Drug- Drug interactions  Core Concepts • Prompt surgical consultation is recommended for patients with aggressive infections associated with signs of systemic toxicity and suspicion for necrotizing fasciitis. • Empiric antibiotic treatment should be broad and initiated early. • The LRINEC is a useful diagnostic adjunct in management to stratify patients who in the low, medium and high risk categories to aid in clinical management. • Goal as an ED physician is to identify these patients, aggressively resuscitate them and get surgery involved quickly. Risk Factors - old, DM, ETOH, immunocompromised, systemic disease (renal, heart, PVD) Classification - Anatomic - Depth - Microbial cause (polymicrobial [type I = most common], monomicrobial [type 2 = strep & staph], vibrio [type 3]) Clinical Features - nec fas is a clinical diagnosis > Pain at site of infection > Blisters/ bullae > Vital sign abnormalities LRINEC - CRP, WBC, Hgb, Na, Cr, Glucose > Low (<5) - prob < 50%, intermediate (6-7) prob 50-75%, High (>8) prob >75% Diagnosis - basic labs, imaging - US, plain films, CT - 80% sensitive, MRI Treatment - OR!!!!! - Antibiotics - PCN & Clindamycin (group A strep) - but cover broadly - vanc + zosyn Teaching points from our surgical colleagues 1. Early diagnosis 2. Early & extensive surgical intervention 3. Life over limb |
Archives
August 2018
Categories
All
|

 RSS Feed
RSS Feed
